
How AHPs Can Use Technology To Improve Patient Engagement
Patients who are actively involved in their health care experience better health outcomes. ‘Patient engagement’ involves strategies to better allow patients to be active participants in their own health care, including providing better information and support about their health condition or needs, and involving them in decision making.
Allied health professionals have a number of different technologies available—many already in use—that can be used to promote and support patient engagement. These include online booking systems, reminders, informative websites and interactive online programs. There are a number of other technologies that are widely in use, such as wearable devices and virtual reality, that have great potential to support patient engagement in allied health, but are less well utilised. This article focuses on a range of technologies that allied health professionals can consider to enhance patient engagement.
Some of these approaches may be beneficial to help meet the needs of patients who are on long waiting lists to access services.
Information provision, support and marketing
Increasingly, allied health service providers are using social media and web portals to market their services and provide educational services to the public or prospective patients.
The clever use of online information provision, combined with search engine optimisation (SEO) for specific conditions can both help prospective patients understand their condition, while providing a referral pathway to your service. For example, a Google search on “managing heel pain” produces a number of informative ‘how-to’ articles (see below). The top SEO positions are held by large, international professional associations, but within the first search results page a number of more localised, podiatry and physiotherapy clinics and services are highlighted due to SEO and Search Engine Marketing efforts.
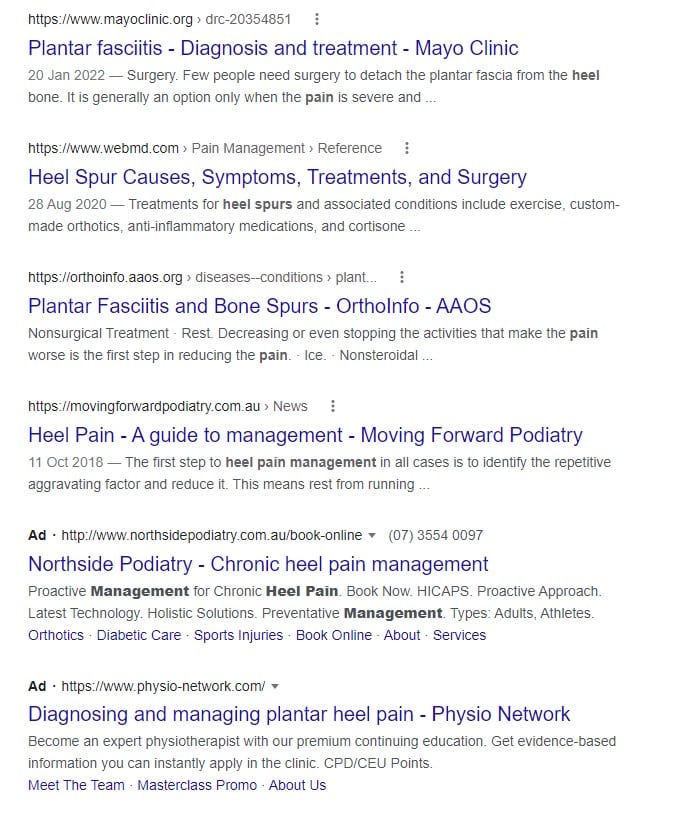
These websites and online resources focus on solving specific problems identified by prospective patients, or issues that arise commonly in the community. High quality, evidence based resources, supported by good web infrastructure can benefit the community—particularly during times of large workforce shortages—but they also provide a level of credibility around the services you provide in your clinic.
Resource libraries
Larger organisations (particularly professional associations) successfully collate a number of patient-centric reports into resource libraries that can be accessed online.
Administration, bookings and automated messaging
Whether managing a public health service or running a private practice, the more time you spend on basic administrative tasks, the less time you have to engage with patients and develop those relationships. Automated messaging services and online booking systems may reduce staff burden and the incidence of human error. Digital patient forms improve communication flow and allow patients time to provide more thorough information.
Online booking services
Anecdotal evidence suggests the rapid growth of online booking systems in health care, however the published research literature needs some new ‘post-COVID’ analysis of how patient behaviour has changed in this regard. Online booking systems can make it easier for patients to access your services, however there is a great deal of complexity around the patient-system-practitioner interaction and outcomes that need more analysis.
Reminder systems
There is now strong evidence to support the use of reminder systems, both as a way to reduce rates of non-attendance at clinics, but also to increase patient adherence to certain treatment approaches and options.
Automated messaging
Automated messaging services are increasingly used to manage patient motivation and adherence to specific interventions. A recent study found that using an automated SMS bot increased adherence to exercise in a group of patients following hip and knee arthoplasty.
Electronic patient records and record sharing
The use of electronic patient records has become ubiquitous in most health care settings. Challenges still remain around the interconnectivity between different service structures and platforms – for instance, being able to access diagnostic test results from different providers.
Technology based treatment approaches
Online interventions
Technology is providing increasing opportunities for people to interact socially, online for health benefits and to improve health literacy. For services with long waiting lists, the provision of group based, online interventions such as courses to help manage falls and balance, where online sessions enable patients to undertake strengthening programs in a group environment. Such activities reduce the risk of social isolation and loneliness and may be considered a form of social prescribing. Therefore, providing online resources improves patient engagement and empowers them to manage their health.
Gamification
Gamification is the use of technologies that increase users’ interactions with digital applications (rather than the passive wearing of devices, for instance). Gamification has been found to have a positive impact on patient engagement with their health behaviours (not necessarily their health practitioner) in a growing number of areas. Gamification is used to increase adherence to medication regimes, management of diabetes, exercise adherence, provide mental health support and improve health literacy.
Group treatment approaches
Online education sessions are not limited to one disease or another. A study demonstrated that delivering diabetes education in a group setting allows for more efficient and cost-effective methods in providing diabetes education programs. In a study evaluating rheumatoid arthritis, researchers reviewed the effectiveness of group education programs in improving the knowledge, behaviour, and health status of patients with this debilitating disease. The researchers warned the effects of group education on health status are rarely maintained in the long run, and further research should develop strategies for maintaining and enhancing early gains from group education. While many group education sessions are run in the traditional face-to-face format, online group sessions are becoming more popular.
Remote service delivery using technology
Using technology outside your workplace is just as important as using it within your practice. The benefit of technology is that it can be used when you are not treating your patient.
Virtual reality
There are increasing opportunities for the use of virtual reality (VR) to support and augment a range of allied health interventions. For example, to help in falls prevention for older people, rehabilitation following acquired brain injury, support for Parkinson’s disease, stroke and cancer. While the evidence is mixed (and preliminary) for many of these interventions, the use of VR appears to have great potential to enhance the engagement of patients in their allied health care.
Telehealth
The provider-patient relationship is vital for several reasons, yet clinic visit time is declining, and administrative tasks are increasing. Such imbalance may result in abbreviated history taking and less thorough assessment. Can patient needs be met under such circumstances? And what of the clinician? For the health professional, there is reduced job satisfaction and risk of burnout when clinic visit time is reduced. The most significant risk is malpractice, especially for specialists managing patients on elective surgical waiting lists, with high patient expectations.
In such situations, innovations such as telehealth have become important. Telehealth improves access for patients who might otherwise be unable to make face-to-face appointments in the clinic. Tele-orthopaedic services allow review of radiographs without patient attendance. Such models have been used in fracture clinics but may also be used for patients on elective surgical waiting lists.
Physiotherapists use telehealth triage and provide assessment and interventions for appropriate patients. Allied health practitioners play a vital role in educating patients on the realities of surgery—recovery times, risks and potential complications. This form of coaching, counselling, support and education rolled into one empowers patients to manage their expectations.
The COVID-19 pandemic has enhanced telehealth’s popularity, providing patients and practitioners more flexible options. Most patients who have used telehealth say they would gladly use it again. While having a screen between you and your patient may seem impersonal, it offers a unique opportunity to engage with the patient when it may not have been possible otherwise. So, rather than allowing the provider-patient relationship to slip, let’s consider how some technologies may improve these relationships.
Remote monitoring
Wearable technologies
Wearable technologies including smart watches and medical grade wearables that monitor vital signs (such as photoplethysmography) have numerous applications in ongoing health monitoring, treatment and early detection. Wearable devices such as Fitbits and Apple Watches can be used to monitor a range of health and lifestyle trends, such as exercise habits, sleep and heart rate. A number of pilot projects are investigating the use of wearable devices to help avoid hospital admissions. Wearable devices are also used to help identify falls risk, monitor gait and mobility after stroke, detect foot pressure in people at risk of ulceration and monitor changes over time resulting from specific interventions.
Service finding directories
Prospective patients need to be able to find your service. While social media offers advertising opportunities, there is more out there. For example, in Australia, HealthDirect now offers a service finder directory – a resource freely available to Australian patients and clinicians. Most professional associations also have a ‘find a practitioner’ service built into their membership portal. Keeping your details accurate and up-to-date will help connect appropriate patients to your service.
Kiosks and portals
Digital information systems, such as touch-screen kiosks and interactive screens have been in use in hospital settings for well over a decade. These are used to help patients navigate complex buildings (like many hospitals), to facilitate contactless service check-in, and can be used to support triage in systems such as hospital emergency departments. The same systems are now being made available on mobile apps for patients to download to allow remote check-in.
Health service and system apps
Some large health departments, such as Queensland Health (“My QH“) have developed phone based apps to help patients manage appointments, provide information about the location of the appointment, and to check-in prior to the appointment. These are particularly useful to help juggle multiple consultations with different providers – as long as all providers use the app.
Targeting patients for specific interventions
Targeted case finding
A more proactive approach to patient engagement that was piloted by the Northern Coast Primary Health Network in New South Wales, Australia involved the interrogation of general practice (GP) patient records by a practice nurse to identify patients with chronic illness who may benefit from a referral to an allied health practitioner.
The project was limited by the variations in GP patient record keeping which hampered accurate case-finding, however those patients that were identified through the case-finding largely benefitted from the direct referral to an allied health practitioner. While only a pilot, this model was believed to have potential to reduce avoidable hospital admissions. This project was funded to undertake the case-finding and also to provide the relevant allied health services.
A similar, pro-active approach may be possible by searching allied health records to identify people at risk of avoidable complications such as falls, diabetes related complications, hearing loss etc.
Conclusion
COVID-19 has created a rapid disruption in the way that health care providers interact with their patients. In addition, staff shortages create an urgent need to rethink the way that health care is delivered to be able to best meet the needs of the community. This article has identified a number of approaches—some of which are tried and tested, others have a great deal of potential to change (and improve) patient engagement with allied health services.
While social media pages allow patients to access the deepest realms of their practitioner’s practice, such as viewing photos and videos, practitioners should not forget that such platforms provide an opportunity for patients to connect in more meaningful ways. Providing patients with clinical advice and linkage to online support groups is perhaps the most potent way technology can improve patient engagement.






